Braces when pregnancy is a topic that many women are concerned about, especially because orthodontic treatment usually lasts from 2 to 3 years. This long treatment period makes many women worry about whether getting pregnant during braces, or starting braces while already pregnant, can affect their health and the health of the baby.
Questions such as: Do X-rays, tooth extractions, interdental expansion, or dental appliances affect the fetus? or Do hormonal changes during pregnancy interfere with orthodontic treatment? are very common. In this article, BeDental will help you clearly understand braces when pregnancy and the three most important things to note for a safe and effective orthodontic journey.
Braces when pregnancy – Is it safe?
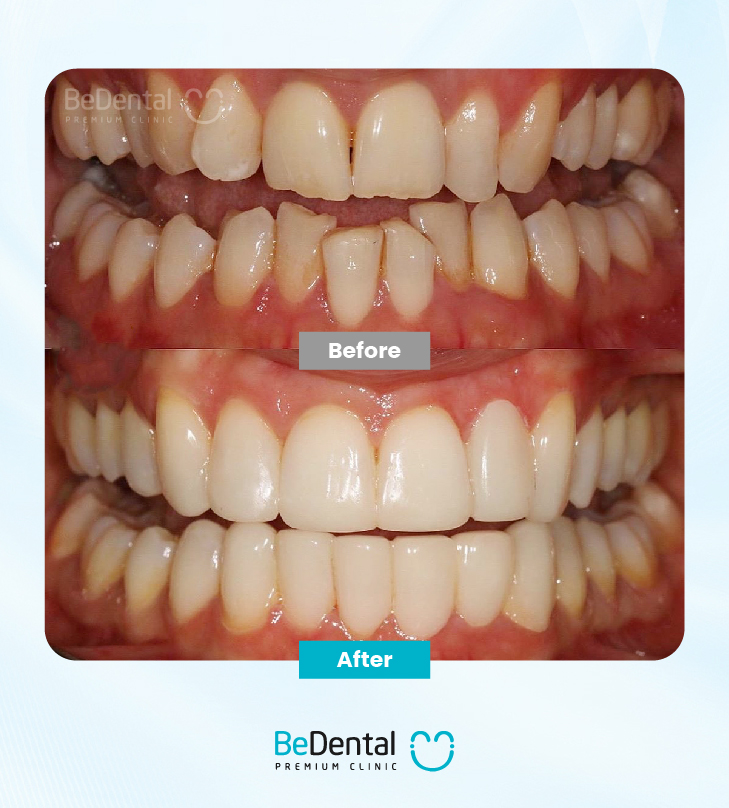
Braces and pregnancy are two completely different issues, but they often overlap in real life. Braces are an orthodontic solution used to correct dental problems such as protruding teeth, underbite, crowded teeth, gaps between teeth, and misaligned bites. Epidemiological studies show that malocclusion affects approximately 60–75% of adolescents and young adults, and about 20–35% require orthodontic treatment for functional or aesthetic reasons. Today, many women choose braces to improve their appearance, boost confidence, and enhance oral health.

However, the duration of orthodontic treatment usually lasts from 18 to 36 months (average ~24 months), and during this time, patients must visit the dentist every 4–8 weeks (some clinics schedule every 2–4 weeks in active phases) for adjustments and check-ups. Each adjustment visit typically lasts 20–40 minutes, while more complex procedures may take 60 minutes or longer. Because pregnancy is also a sensitive and demanding period lasting about 40 weeks, many women hesitate to start braces or decide to postpone treatment. On the other hand, some women take advantage of 6 months of maternity leave (common in Vietnam) to begin orthodontic care, while others unexpectedly become pregnant in the middle of their braces journey. This leads to the big question: Is it safe to wear braces when pregnant?
In principle, braces do not directly affect pregnancy. Orthodontic treatment involves applying light, continuous forces of approximately 50–150 grams to gradually move teeth through bone remodeling. These forces act locally within the periodontal ligament (typically 0.2–0.4 mm thick) and alveolar bone, without affecting internal organs or the reproductive system. Clinical evidence indicates that orthodontic appliances themselves pose no direct risk to the fetus, and there is no scientific data showing increased miscarriage or fetal abnormality rates due to braces.
However, the orthodontic process may involve additional procedures that require caution during pregnancy. For example:
- Dental X-rays: Modern digital dental X-rays expose patients to very low radiation levels (approximately 0.005–0.01 mSv per image), which is far below the 50 mSv threshold associated with fetal risk. With protective lead aprons and thyroid collars, exposure to the fetus is considered negligible.
- Tooth extraction (if required): About 20–50% of moderate-to-severe orthodontic cases may require premolar extraction. The safest period for necessary dental procedures during pregnancy is the second trimester (weeks 14–27).
- Pain management: Mild discomfort after tightening typically lasts 2–5 days. Acetaminophen (paracetamol) is generally considered safe during pregnancy when used at recommended doses, whereas some NSAIDs are restricted, especially in the third trimester.
Additionally, pregnancy causes hormonal changes—particularly increased estrogen and progesterone levels (up to 10–30 times higher than normal)—which can increase blood flow to gum tissue and raise the risk of pregnancy gingivitis. Studies suggest that 60–75% of pregnant women experience some degree of gingival inflammation, and braces may further increase plaque retention by 20–30% if oral hygiene is not maintained properly. Hormonal changes may also slightly influence bone metabolism, potentially affecting the rate of tooth movement.
In summary, wearing braces during pregnancy is generally safe, but it requires careful planning, close communication between the orthodontist and obstetrician, and stricter oral hygiene control to minimize indirect risks.
See more: Braces near me in Vietnam
Should you get braces during pregnancy?

So, should you get braces when pregnant? The answer is yes, it is possible, but it is not always recommended. Pregnancy lasts around 38–40 weeks (about 9 months), while comprehensive orthodontic treatment typically requires 18–36 months (average ~24 months). This means pregnancy covers only about 25–40% of a full braces treatment cycle.
If you are already pregnant and planning to start braces, most dentists suggest waiting until after childbirth. The first trimester (weeks 1–13) is the most sensitive stage of fetal development, when major organs form, and dentists generally try to avoid elective procedures during this period. Although orthodontic appliances themselves are safe, the initial stage of braces may involve:
- Diagnostic X-rays (even though digital dental X-rays are very low dose, about 0.005–0.01 mSv per image, far below the 50 mSv fetal risk threshold)
- Possible tooth extraction in moderate-to-severe cases (20–50% of such cases may require extraction)
- Initial soreness lasting 3–7 days after appliance placement
Because pregnancy is already associated with increased fatigue (reported in over 70% of pregnant women, especially in the first trimester), nausea, and hormonal fluctuations, adding orthodontic discomfort may increase physical and emotional stress.
The postpartum period is often more suitable for starting orthodontic treatment because hormonal levels (estrogen and progesterone, which can rise 10–30 times above normal during pregnancy) gradually stabilize after delivery. Gum inflammation, which affects 60–75% of pregnant women, also tends to improve after childbirth. A more stable hormonal and immune condition may support better oral hygiene and more predictable tooth movement.
Starting braces after pregnancy can also reduce the burden of frequent appointments. Orthodontic patients usually require check-ups every 4–8 weeks, meaning about 6–12 visits per year. During late pregnancy, mobility may be limited, and prolonged supine positioning in the dental chair can cause discomfort due to pressure on the inferior vena cava.
However, if you are already wearing braces before pregnancy, there is usually no need to remove them. Research and clinical consensus indicate that orthodontic treatment does not increase the risk of miscarriage, preterm birth, or fetal abnormalities. As long as:
- Your pregnancy is medically stable
- You maintain good oral hygiene (braces can increase plaque retention by 20–30%)
- Your orthodontist adjusts treatment plans conservatively
you can safely continue treatment throughout pregnancy.
Three important things to note about braces when pregnancy

| Key Factors | First Trimester (Weeks 1–13) | Second Trimester (Weeks 14–27) | Third Trimester (Weeks 28–40) |
| Physiological & Hormonal Changes | – Organogenesis (major fetal organ formation) occurs.
– Estrogen & progesterone levels may increase 10–30 times above normal. – 60–75% of pregnant women develop pregnancy gingivitis. – Up to 70% experience nausea and fatigue. |
– Hormonal levels relatively more stable.
– Reduced nausea and improved appetite. – Blood circulation remains elevated, increasing gum sensitivity. |
– Rapid fetal growth increases abdominal pressure.
– Higher risk of supine hypotensive syndrome when lying flat. – Increased fatigue, shortness of breath, and back pain. |
| Starting Orthodontic Treatment | ❌ Generally not recommended. Elective procedures should be postponed. Avoid unnecessary X-rays or extractions. | ✅ Safest period if orthodontic care is necessary. Diagnostic procedures can be performed with proper shielding. | ⚠️ Not ideal to begin new treatment due to physical discomfort and limited mobility. |
| Continuing Existing Braces | – Can continue with lighter forces (50–100g range).
– Avoid aggressive adjustments. – Monitor gum inflammation closely. |
– Treatment can proceed normally with careful periodontal monitoring.
– Scaling and professional cleaning may be performed if needed. |
– Consider shortening appointments.
– Avoid long procedures (>30–40 minutes supine). – In rare high-risk medical cases, temporary removal may be discussed. |
| Gum & Oral Health Risk | – Increased vascularity leads to gum swelling and bleeding.
– Braces may increase plaque retention by 20–30%. – Higher risk of localized gingival hyperplasia. |
– Gingivitis risk persists but is more manageable with good hygiene.
– Periodontal monitoring is important. |
– Continued risk of inflammation if oral hygiene declines due to fatigue. |
| Recommended Oral Care | – Brush ≥2 times/day with soft bristles. – Fluoride toothpaste ~1000 ppm. – Interdental brushes and floss mandatory. – Alcohol-free antimicrobial mouthwash. | – Maintain strict hygiene routine. – Warm saline rinse can soothe inflamed gums. – Professional cleaning if plaque accumulates. | – Maintain consistent hygiene habits. – Check for loose brackets or wires before delivery. |
| Medical & Clinical Concerns | – First trimester is most sensitive for fetal development. – Dental X-rays: 0.005–0.01 mSv per digital image (far below 50 mSv risk threshold). – Stress management is crucial. | – Considered safest window for dental procedures. – Local anesthesia without vasoconstrictor may be preferred depending on obstetric advice. | – Avoid prolonged supine position due to vena cava compression. – Rare anesthesia risk if loose brackets during emergency intubation. – Resume orthodontic monitoring soon after childbirth to prevent relapse. |
Are braces painful?
One of the most common questions women ask dentists is: Are braces painful? In reality, braces do not cause unbearable pain, but they do create temporary discomfort, pressure, and sensitivity—especially in the early stages.
Clinical studies measuring orthodontic pain using the Visual Analog Scale (VAS, 0–10 scale) show that most patients report discomfort at a level of 3–6/10, which is considered mild to moderate pain. The discomfort typically:
- Begins 4–6 hours after adjustment
- Peaks at around 24–48 hours
- Gradually decreases within 3–7 days
Only a small percentage of patients (about 5–10%) report severe pain (≥7/10).
| Procedure | How It Feels | Prevalence of Discomfort | Peak Discomfort | Duration of Symptoms | Recovery / Adaptation |
| Elastic Separators (Spacers) | Soreness and pressure between teeth, similar to food being stuck | 60–80% of patients report mild discomfort | Within 24 hours | 2–5 days | Usually resolves on its own without medication |
| Tooth Extraction (if required) | Mild to moderate pain at extraction site, possible swelling | 20–50% of orthodontic patients require extraction (moderate–severe cases) | Swelling peaks at 48 hours | Pain lasts 1–3 days | Most patients return to normal function in 3–5 days; pain controlled with approved medication (e.g., acetaminophen) |
| Bracket & Wire Placement | Tightness, pressure on teeth; irritation to cheeks and lips | 70–90% experience initial soreness | 24–48 hours after placement or adjustment | 2–4 days after each adjustment | Most adapt within 2–4 weeks; discomfort decreases as treatment progresses |
Why Choose BeDental for Braces in Vietnam?

Specialized Orthodontic Expertise at BeDental
Orthodontic treatment at BeDental is led by certified specialists experienced in both routine alignment and complex bite correction. Each treatment plan is customized based on facial structure, dental condition, bite function, and lifestyle needs—rather than applying a one-size-fits-all approach.
Malocclusion affects approximately 60–75% of adolescents worldwide, with 20–30% requiring comprehensive orthodontic care. BeDental’s team is trained to manage cases ranging from mild crowding to severe malocclusion, including deep bite, open bite, and crossbite.
Transparent Pricing and Long-Term Treatment Support
BeDental applies an international-standard cost management model, helping patients clearly plan their orthodontic investment. Most services are eligible for dental insurance coverage (depending on individual policies).
The clinic also offers interest-free installment plans, making long-term orthodontic treatment more financially accessible—especially for students and working professionals.
After treatment, structured retention programs are provided. Regular follow-ups and professional retainer guidance help prevent relapse, ensuring long-term stability of results.
Dedicated Care for International Patients
BeDental supports overseas patients through online consultations and multilingual assistance throughout the treatment process.
Flexible scheduling allows patients to coordinate appointments with travel plans while maintaining continuity of care. With cross-border dental demand increasing by 15–20% annually, BeDental’s organized coordination system ensures predictable treatment outcomes for both local and international patients.
Conclusion
Braces when pregnancy is not a taboo, but it requires careful consideration and professional guidance. Orthodontic treatment does not directly harm the fetus, but pregnancy-related factors such as hormonal changes, fatigue, and medical risks can influence the braces process.
The most important things to remember are to consult your dentist and obstetrician, maintain excellent oral hygiene, avoid invasive procedures during sensitive stages, and prioritize your health and comfort. If possible, starting braces after childbirth is often the safest and most convenient option.
Hopefully, this article has helped you better understand braces when pregnancy and provided useful knowledge for women who are planning orthodontic treatment. If you have more questions about dental services, such as wisdom tooth extraction costs or installment payment options, feel free to contact BeDental for professional advice and support.
See more: Does getting braces hurt? Which stage is the most painful?


 English
English 한국어
한국어 日本語
日本語 中文 (中国)
中文 (中国)